Patients harmed as NHS neared collapse during Covid pandemic, inquiry reveals
Patients experienced harm as the NHS approached collapse in the UK amid the Covid pandemic, according to findings from the Covid inquiry.
The third report, one of ten planned by the ongoing inquiry, concluded that the health service "only just coped" with the unprecedented crisis.
The report depicted NHS staff working under conditions described as "war zones" and highlighted how patients were unable to receive necessary care as hospitals and ambulance services struggled to manage the surge in Covid cases.
It also criticised the NHS's fragile state at the pandemic's outset and suggested that the government slogan "Stay Home, Protect the NHS, Save Lives" may have inadvertently caused harm by discouraging individuals with other health issues from seeking medical assistance.
"We coped, but only just. Collapse was only narrowly avoided thanks to the extraordinary efforts of all those working in health care," said inquiry chair Baroness Hallett.
The inquiry emphasised that to effectively manage any future pandemics, there must be greater capacity to rapidly expand hospital and ambulance services.
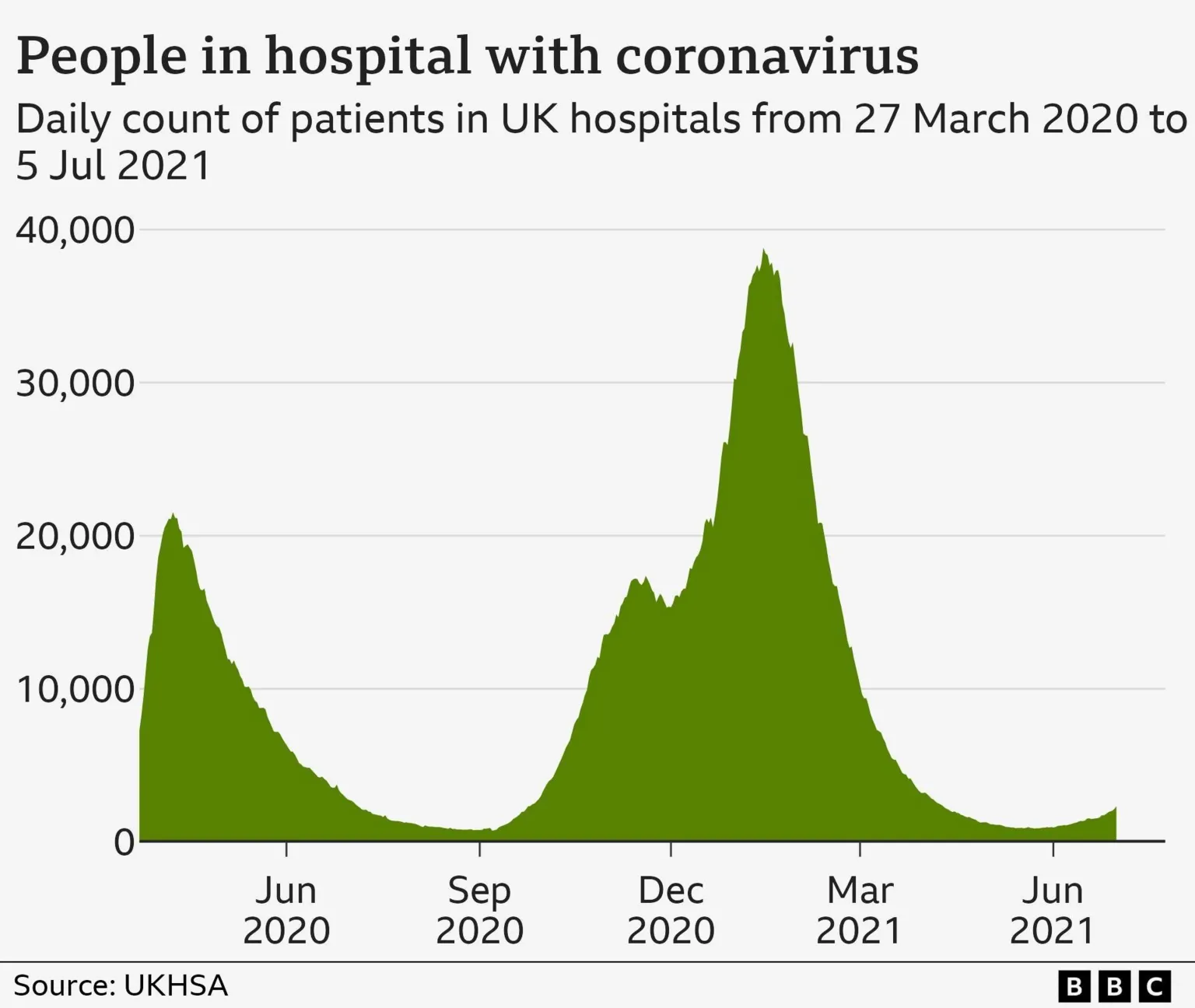
Intolerable pressure on NHS during pandemic waves
Between March 2020 and May 2023, nearly 227,000 people died from Covid in the UK, a period that concluded when the World Health Organization declared the "global health emergency" over.
The report, spanning over 400 pages, detailed the intolerable pressure faced by the NHS as it confronted successive waves of Covid infections.
It highlighted a notable decline in attendances at Accident & Emergency departments and other healthcare settings for non-Covid emergencies, including heart attacks. This suggested that the "Stay Home, Protect the NHS, Save Lives" message unintentionally conveyed that healthcare services were unavailable.
Additionally, the widespread cancellation of non-urgent care procedures, such as knee and hip replacements, was found to have a "debilitating effect" on patients' quality of life and mobility.
Tough restrictions and their consequences
Visiting restrictions implemented during the pandemic left some vulnerable patients, including women in labour and individuals with disabilities, without essential support. The inquiry recommended avoiding such stringent rules where possible in future crises.
These restrictions also caused profound distress among bereaved family members, who experienced feelings of heartbreak, guilt, and anger as their loved ones died alone.
The report noted that supplies of personal protective equipment (PPE) reached "dangerously low" levels, with the NHS reportedly only days away from running out of critical items at one point.
Staff endured significant psychological trauma, with some describing their work environments as "war zones," leading to cases of post-traumatic stress disorder.
Staff impact and ongoing challenges
Dr Tom Dolphin of the British Medical Association stated that many healthcare workers "tragically paid with their lives" due to systemic failings. Research indicates that health workers experienced higher excess mortality in the first year of the pandemic compared to other professions.
He further noted that this impact disproportionately affected ethnic minority staff.
"The impact on doctors and our colleagues was stark, as painfully recounted in this report," Dolphin added.
He also warned that the NHS remains "over-stretched" and "under-staffed" to this day.
The Covid-19 Bereaved Families for Justice described the report as "utterly damning."
"Our loved ones, many of whom were healthcare workers themselves, paid with their lives. Years of austerity left the NHS dangerously exposed, without the staff, beds or resilience needed to withstand a major shock."
Layla McKay, representing NHS Confederation and NHS Providers, which advocate for hospitals, stressed the importance of translating these lessons into action.
"It is vital that these lessons translate into meaningful action, strengthened preparedness and a more resilient health and care system for the future."






