Warning: Mental Health Struggles Discussed
This story contains discussion of mental health challenges including self-harm and suicidal thoughts.
Naomi Durnham's Experience with Diabetes and Depression
A woman living with type 1 diabetes has spoken about feeling that her two young daughters "would be fine if they didn't have me" during her battle with depression.
Naomi Durnham, 34, from Cardiff, experienced severe post-natal depression following the birth of her second daughter during the Covid-19 pandemic.
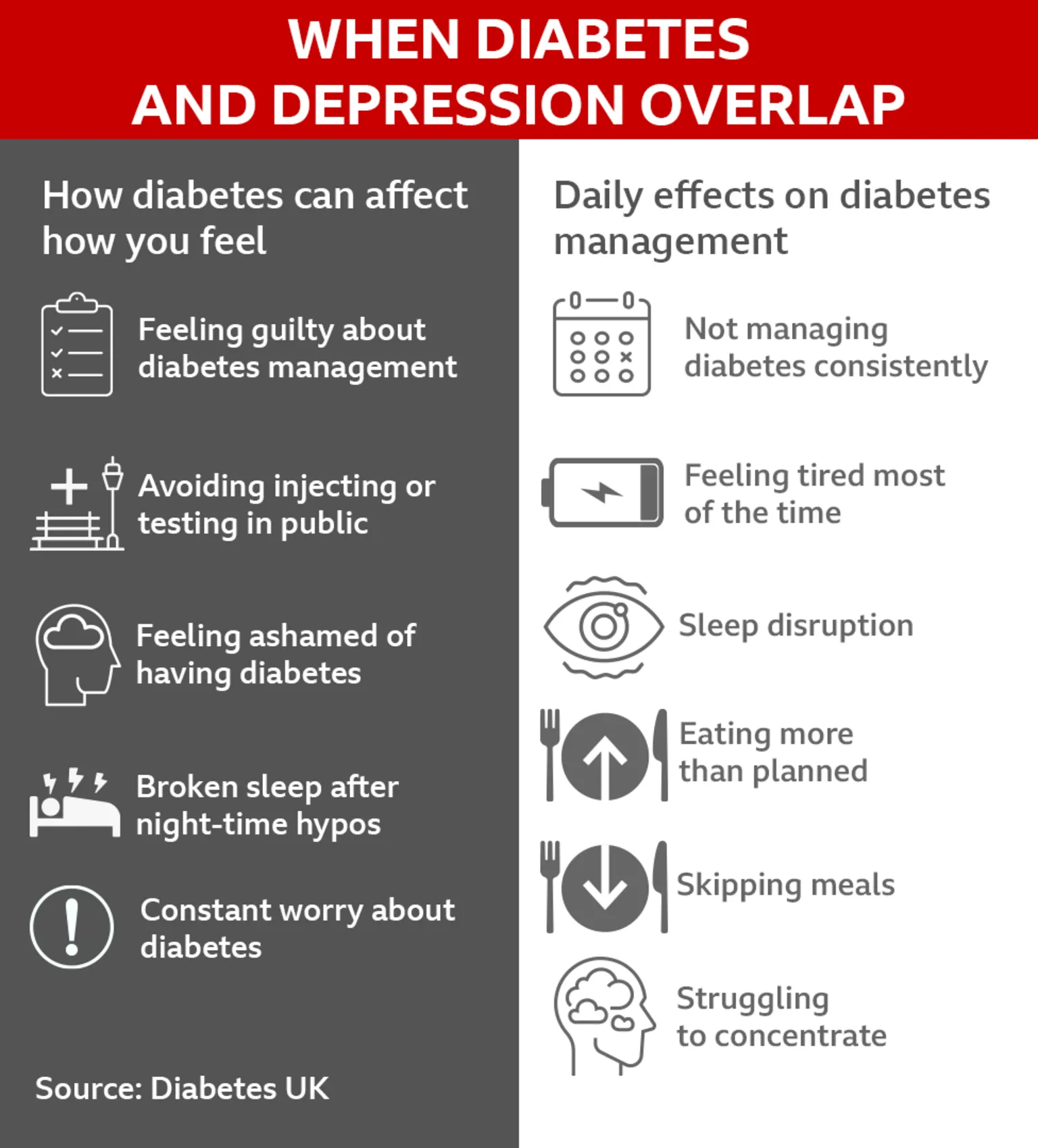
Diabetes UK reports that individuals with diabetes, a condition affecting blood glucose levels, are twice as likely to experience depression. The overlap in symptoms between diabetes and depression can complicate access to appropriate support.
A leading diabetes psychology expert, who is developing a pioneering UK care pathway, described managing diabetes as akin to "having to beat your own heart".
Cardiff and Vale University Health Board stated it provides a perinatal mental health service that offers "specialist, safe, effective and compassionate care." The board expressed regret over Naomi's experience and, while unable to comment on individual cases, encouraged her to contact its concerns team.
Naomi recounted spending much of the lockdown period feeling "completely numb."
"My health visitor was amazing, she could see I wasn't myself and she thought I needed some more support so she contacted my GP on my behalf,"
she said.
However, Naomi said her GP prescribed increasing doses of anti-depressant medication over the phone without face-to-face consultations, eventually reaching the maximum dose. There was no indication that perinatal mental health support was offered.
"I wasn't really feeling any benefit from it at all,"
she added.
At her lowest point, Naomi neglected to take the insulin required for managing her type 1 diabetes.
"I just didn't care about myself... I had complete lack of self worth, I didn't feel like I needed to be here anymore,"
she said.
She developed diabetic ketoacidosis (DKA), a life-threatening condition caused by insufficient insulin leading to acidic blood, resulting in numerous hospital admissions.
Naomi felt there was insufficient support addressing both her mental health and diabetes management.
"The diabetes team would say it was mental health, and the mental health team would say it was a diabetes problem,"
she recalled.
"Those two worlds collide because there's no services set up for that."
Over two years, Naomi was repeatedly hospitalized, which forced her to discontinue her nursing studies. At one point, concerns arose about her ability to care for her children.
She credited peer support networks, including online communities, single parent groups, and charity services, with aiding her recovery and enabling her to resume her education. Nevertheless, she remains concerned about the long-term effects on herself and her daughters.
"It took a long time to admit that I needed help,"
she said.
"I felt guilty that I wasn't there for the girls... I am so conscious of damaging them."
Naomi acknowledged the limited time GPs have but emphasized that repeatedly advocating for herself exacerbated her difficulties. She called for more holistic assessments and appropriate signposting to available support.

Duke Al's Story: Managing Type 1 Diabetes and OCD
Spoken word poet Duke Al, 32, from Sully, Vale of Glamorgan, was diagnosed with type 1 diabetes at age 23 in 2018.
He praised the diabetes nurses who taught him insulin injection techniques as "fantastic... really gentle and caring," and initially coped well with the diagnosis.
However, over time, he experienced growing frustration and struggled with feelings of being "a weaker version of myself."
"That very quickly turned into self-destruct mode, where I would neglect insulin, I deliberately wouldn't inject, which can be very dangerous."
Duke, who has obsessive compulsive disorder (OCD), described how the diabetes diagnosis dramatically exacerbated his mental health challenges.
His OCD manifests as intrusive thoughts related to numbers and repetitive behaviors performed to prevent perceived negative outcomes. Uncertainty plays a significant role in this condition.
"It's like this super-glued grip on your brain is like, if you don't do that compulsion, what if this thing does happen and it's your fault?
Even though I know it's irrational, that's the nature of the condition."
At its worst, Duke would inject incorrect insulin doses to avoid confronting "bad numbers."
He struggled significantly for about a year and occasionally since then.
Duke explained that diabetes burnout can occur when managing blood glucose, insulin injections, diet, and exercise becomes overwhelming.
Currently, he reports being "in a good place" but noted limited mental health support was available.
"First and foremost, my coping mechanism is poetry. I use poetry as a self-therapy to express how I feel,"
he said.
"I didn't want to tell anybody about how I was feeling in fear of stigmatisation and fear of not being understood. My brain told my hand, my hand told the pen, the pen told the page and I was able to figure out what was going on and articulate myself really well.
It's a way of reaching other people, hopefully raising awareness, and connecting through creativity."
He is advocating for increased psychological support for individuals living with type 1 diabetes.
"Even though your numbers or your HbA1c might read fantastic and your blood glucose are in range, that doesn't mean you're always feeling well mentally.
I think the person needs to be treated as the whole."
Developing Integrated Care for Diabetes and Mental Health
Dr Rose Stewart, diabetes psychology lead for Wales, highlighted the significant mental health impact of living with diabetes.
"A lot of people compare it to having to beat your own heart. It's something that you never get to switch off from,"
she said.
She referenced recent research demonstrating a "bi-directional relationship" where mental health issues impair self-care behaviors, leading to diabetes complications, which in turn worsen mental health.
Dr Stewart frequently encounters patients caught between diabetes and mental health services, with neither equipped to address their combined needs.
"It's something that we're working really hard in Wales to rectify,"
she stated.
Within NHS Wales' performance and improvement unit, Dr Stewart is developing a national diabetes psychology pathway to provide rapid access to specialist support tailored to individual needs, including online programs, individual therapy, and crisis care.
"This is the first to exist in the UK, and possibly in the world, looking at developing an entire model of care for people living with diabetes,"
she explained.
"This won't just be about people having access to psychology and therapy rooms, this will be about upskilling our diabetes staff."

Political Responses and Calls for Improved Services
Reform UK emphasized the importance of mental health services addressing the specific challenges faced by people with diabetes.
The Green Party expressed support for "more joined‑up, accessible mental health provision for people living with long term conditions such as diabetes."
The Conservative and Liberal Democrat parties acknowledged the difficulties experienced by people with diabetes and backed "better integration" of physical and mental health services.
Plaid Cymru pledged to tackle "the social determinants of mental health... by ensuring that the public and third sectors work effectively together" if elected.
Labour has been approached for comment.
Support Resources
If you have been affected by the issues discussed in this story, help and support are available via BBC Action Line.






